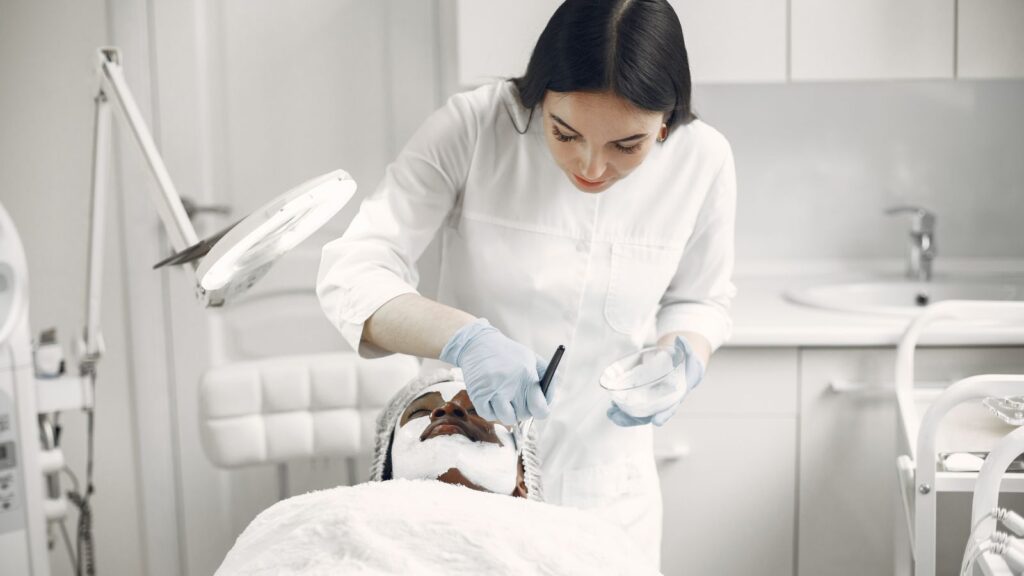
Modern aesthetic treatments rely far less on products than many patients assume. The visible result of an injectable or skin procedure is determined mainly by the training behind the hands delivering it. As non surgical aesthetics has grown into a multibillion dollar global industry, the gap between well trained practitioners and minimally trained providers has become one of the most important safety issues for patients. Regulatory bodies, insurers, and professional associations now point to education quality as the single strongest predictor of safe outcomes in aesthetic medicine.
Clinical data supports this shift. A 2022 review published in Aesthetic Surgery Journal found that over 70 percent of reported filler related complications were linked to improper injection technique or poor anatomical knowledge rather than product defects. These findings explain why training has moved away from short workshops and toward structured programs that emphasize anatomy, risk recognition, and evidence based decision making. For patients, this means treatment quality depends directly on the depth and recency of a provider’s education.
Why Proper Training Directly Impacts Patient Safety
Facial anatomy is complex and highly variable. Major blood vessels such as the facial artery angular artery and infraorbital artery can sit at different depths depending on age sex and facial structure. Cadaver studies published in Clinical Anatomy show that arterial depth in the midface can vary by more than 5 millimeters between individuals. Without training that addresses this variability, even experienced clinicians face elevated risk.
Vascular occlusion remains the most serious complication associated with dermal fillers. While overall incidence is low, estimated at roughly 1 in 6,000 to 1 in 10,000 syringe uses, outcomes depend entirely on response speed and accuracy. A multicenter study analyzing 98 vascular occlusion cases found that providers who had completed formal complication management training achieved tissue recovery in over 85 percent of cases. Providers without structured training showed significantly higher rates of necrosis and scarring.
Training also affects patient assessment. Facial aging does not follow a single pattern. Research using three dimensional imaging has demonstrated that volume loss occurs unevenly across fat compartments rather than uniformly. Practitioners trained in compartment based anatomy place filler more conservatively and avoid overcorrection. This approach reduces long term complications such as product migration and unnatural contouring which often appear months after poorly planned treatments.
What Comprehensive Aesthetic Training Actually Includes
High quality aesthetic education follows a defined structure. Theoretical instruction typically covers facial anatomy neurovascular mapping and skin physiology. Advanced programs include ultrasound anatomy training which allows practitioners to visualize vessels and filler placement in real time. A 2021 controlled study showed that clinicians trained with ultrasound guidance reduced intravascular injection risk by over 60 percent compared with those trained using surface anatomy alone.
Hands on training progresses in stages. Simulation models are used first to practice injection angles depth control and pressure management. These models replicate tissue resistance and allow objective evaluation of technique. Live patient training follows under direct supervision with standardized assessment tools such as injection mapping and post treatment outcome scoring.
Complication management is no longer treated as optional. Modern curricula include step by step protocols for vascular compromise delayed inflammatory nodules and biofilm related reactions. Hyaluronidase dosing algorithms are taught using case based learning. Providers trained under these models demonstrate faster intervention times and better resolution outcomes according to data collected by medical indemnity insurers.
Ethical decision making forms another core element. Training emphasizes patient selection contraindications and realistic outcome counseling. Long term follow up studies show that practitioners who decline inappropriate treatments experience lower complaint rates and higher patient retention. This aspect of training directly affects both safety and trust.
Dermal Filler Training Resources and Evidence Based Learning
How Dermal Filler Training Resources Shape Clinical Competence
Access to structured learning materials has changed how practitioners maintain competence. dermal filler training resources provide on demand education that reflects real clinical scenarios rather than idealized demonstrations. These resources often include full procedure recordings complication case reviews and anatomical dissections which allow practitioners to study outcomes over time.
Retention studies conducted by continuing medical education providers show that video based learning combined with case analysis improves long term knowledge retention by approximately 40 percent compared with single day workshops. This matters because aesthetic complications often occur months after treatment. Providers who understand delayed reactions such as granulomatous inflammation are better prepared to manage them effectively.
Professional insurers increasingly reference documented training when evaluating coverage eligibility. Claims data from medical indemnity providers indicate that clinicians with documented ongoing education file significantly fewer high severity claims. As a result many insurers now require proof of updated training every one to two years for injectable coverage.
Structured resources also promote consistency across disciplines. Physicians nurses and dentists enter aesthetic medicine with different baseline training. Standardized educational materials create a shared clinical language which improves team based care. Clinics using unified training frameworks report fewer treatment errors and improved patient satisfaction metrics according to internal audit data published by large provider networks.
How Ongoing Training Improves Long Term Outcomes
Aesthetic medicine evolves quickly. Product rheology injection devices and safety protocols change as new evidence emerges. Providers who engage in ongoing education adapt faster and practice more conservatively. Longitudinal data tracking complication rates over five years shows a steady decline among practitioners who complete annual refresher courses compared with those who do not.
Continued training also affects dosing strategy. Studies examining repeated filler treatments demonstrate that lower volume maintenance approaches preserve tissue quality better than large volume intermittent treatments. Providers trained on long term tissue behavior adjust treatment plans accordingly which reduces fibrosis and irregular texture.
Patient communication improves with education. Trained practitioners explain risks timelines and limitations with greater clarity. Surveys conducted across aesthetic clinics reveal that patients who feel well informed report higher satisfaction even when changes are subtle. This correlation highlights how education influences perception as much as physical outcome.
Follow up protocols also benefit from structured learning. Evidence based training encourages standardized photography outcome scoring and documentation. These practices allow early identification of issues and timely intervention. Clinics that implement structured follow up report lower rates of unresolved complications and higher repeat visit rates.
Training behind modern aesthetic treatments shapes safety outcomes clinical confidence and patient trust at every stage of care. As demand for non surgical procedures continues to rise the importance of well structured evidence based education becomes increasingly clear. Patients benefit most when providers invest in training that reflects both current science and real world clinical complexity.